Doctors moonlight as medical tech inventors
By Tara Deschamps, The Canadian Press, Toronto
Electronics Engineering Medical medical medical tech techCanadian health care system faces unique hurdles to commercialization of these types of products
In Dr. Joao Rezende-Neto’s 25-year career as a trauma surgeon, he’s only twice dealt with patients who insisted on forking over big bucks to buy equipment for a procedure. 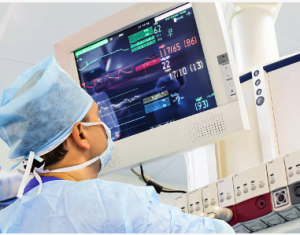
One instance occurred in Brazil, where medical technology is far less advanced, and his patient needed a tracheostomy – a procedure involving an incision made in the windpipe to clear breathing obstructions. The patient’s family was so intent that the procedure be done with a specific device that minimizes the incision that they shelled out $5,000 to have the equipment imported.
“In my trauma centre we had 10,000 traumas a year and every week we did 10 or 15 tracheostomies,” Rezende-Neto recalled. “I thought this is unfair. Why can’t we have this (device) for everyone?”
Getting it approved and commercialized has come with challenges
The incident was so powerful that Rezende-Neto invented a device to make such procedures more efficient and less expensive. However, getting it approved and commercialized has come with challenges – a hallmark of the clinical medicine field.
Experts say the sector is ripe for technology, but doctors are often pushed towards research instead of entrepreneurship, and can find themselves lacking funding and support, leaving ideas for more efficient devices and cost-saving innovations unrealized.
In the age of hallway medicine, patients and the Canadian health care system are left to pay the price. A 2016 Industry Canada study showed the country exports about $3.1 billion in medical device technology, including pacemakers, surgical tools and catheters, but imports far more – about $8.6 billion.
“To get a (medical) idea to a final product is extremely complicated and the hurdles are very high,” Rezende-Neto said. “Maybe doctors are discouraged to carry on and give up when they hear about the approvals you have to do.”
Provide guidance, support and access to doctors to health technology startups
For Rezende-Neto to get his device closer to market, he started a company called Inventorr with St. Michael’s Hospital surgeon-in-chief Ori Rotstein and entrepreneur Chris Bass. They successfully tested their device in humans and animals, but still felt the need to turn to the Biomedical Zone, a four-year-old partnership between St. Michael’s and Ryerson University in Toronto, which aims to provide guidance, support and access to doctors to health technology startups.
Among the dozens of companies it has supported are Pilly, a prescription delivery service; RetiSpec, the creator of a tool for detecting Alzheimer’s disease through the eyes; Marion Surgical, which makes a virtual reality surgery simulator; and HelpWear Wearable Technologies, which invented a what does this mean? electrocardiogram that can be worn on a wrist or arm.
Dr. Linda Maxwell, the zone’s founding director and a plastic surgeon, is adamant about startups she courts needing to have a clinical focus because of resistance it faces.
“The culture is changing, but it has not necessarily been one to want to embrace a lot of newness (because) we don’t want risk and we want to minimize risk because we want patients to always do well,” she said.
Joseph Ferenbok, the co-director of the University of Toronto’s Health Innovation Hub, said doctors who choose to be entrepreneurial know it will be harder for them to receive grants in an increasingly competitive and under-funded sector if they are not producing results quickly. Few, he said, would step away from their jobs for the uncertainty that comes with a startup, especially when most don’t have a business background.
But it’s people like doctors and medical professionals that health tech businesses need, he said.
“(If you are a startup), you can’t stand outside a hospital and solicit information from people you think are patients coming out and you can’t go into a ward and make sure you understand exactly the nature of the problem unless you have access like a clinician or researcher,” he said.
Those who do have access can still struggle, he said, as medical policies are prone to shifting frequently.
“Deep science takes a lot of time to get out and a lot of money and it takes a lot of knowledge. It is not like an app where you will get a return in six months,” he said.
“I am not sure we are going to be experts in making huge companies that do a lot of manufacturing because we are a small market and (startups) don’t have other companies to work with here. We are the incubators of ideas and companies and what we should be thinking about is how do we help these ideas incubate and sell off their products and intellectual property to others that are bigger globally but retain the talent and knowledge.”
Supporting entrepreneurial medical professionals
Retaining that talent and knowledge is also a fixation for Maxwell, who considers Rezende-Neto – who has 13 other ideas for medical devices, including a cardiac plug already in development that allows for easy temporary hemorrhage control from wounds to the heart – a rarity that she desperately wants to change.
She’s also keen on supporting entrepreneurial medical professionals as a way to tackle a common lament in Canada’s tech scene: the growing number of companies that get acquired by American firms or migrate to the U.S., taking Canadian innovation and talent with them.
“It takes so long to get things to get to market and it is so expensive that for small- or even medium-sized companies, they just cannot survive in Canada,” she said. “If we want to keep our Canadian companies here, they need a lot more support around them than what we currently do.”